Factsheet for health professionals about dengue
Dengue is a mosquito-borne viral disease widely spread in tropical and subtropical regions. The disease is transmitted by Aedes mosquitoes, which breed in a peri-domestic environment. While most of the clinical cases present a febrile illness, severe forms including haemorrhagic fevers and shock with fatalities have been reported as well. The disease is under European Union (EU) surveillance. It is by far the most important mosquito-borne viral disease affecting humans worldwide. Tens of millions of cases occur each year resulting in approximately 20 000–25 000 deaths, mainly in children.
There are four serologically distinct dengue viruses, so people living in a dengue-endemic area can have several dengue infections in their lifetime. Dengue is endemic in most of the European Overseas Countries and Territories (OCTs) located in tropical areas. Limited outbreaks may occur in continental Europe, in areas infested by the Aedes albopictus, an invasive mosquito species that has spread over the past twenty years.
Case definition
Clinical criteria
Fever
Laboratory criteria
1. Probable case
— Detection of dengue-specific Immunoglobulin M (IgM) antibodies in a single serum sample.
2. Confirmed case
At least one of the following five characterisations:
— Isolation of a dengue virus from a clinical specimen;
— Detection of dengue viral nucleic acid from a clinical specimen;
— Detection of dengue viral antigen from a clinical specimen;
— Detection of dengue-specific IgM antibodies in a single serum sample;
AND
Confirmation by neutralisation;
— Seroconversion or four-fold antibody titre increase of dengue-specific antibodies in paired serum samples.
Epidemiological criteria
History of travel to, or residence in an area with documented on-going transmission of dengue, within a two-week period prior to the onset of symptoms.
Case classification
1. Possible case NA
2. Probable case
Any person meeting the clinical and the epidemiological criteria, and the laboratory criteria for a probable case.
3. Confirmed case
Any person meeting the laboratory criteria for a confirmed case.
The pathogen
- Dengue is caused by a virus of the Flaviviridae family, Flavivirus genus, which includes viruses such as yellow fever virus, West Nile virus (WNV), and tick-borne encephalitis (TBE) virus.
- There are four distinct dengue viruses without cross immunity. As such, people can have up to four dengue infections in their lifetime.
Clinical features
- Up to 80% of all dengue infections are asymptomatic.
- Commonly reported clinical symptoms include
- sudden onset of high fever
- severe headache and retro-orbital pain
- myalgia
- arthralgia
- maculopapular rash
- minor haemorrhage.
- Fever and other symptoms often follow a ‘saddleback’ sequence, with a brief remission after the third day. The illness rarely lasts for more than 10 days, but convalescence can be prolonged and debilitating.
- A portion of cases, usually < 5%, can be severe and a fraction of these may be fatal. Most severe cases and fatalities occur among children and adolescents. Severe dengue — commonly referred to as ‘dengue haemorrhagic fever / dengue shock syndrome (DHF/DSS)’ to distinguish it from ‘classic’ dengue fever (DF) — is characterised by an increase of vascular permeability that can lead to life-threatening hypovolemic shock.
- The causes of the severe dengue (DHF/DSS) condition have been debated for decades, but remain unresolved. A hotly contested hypothesis is that after a ‘primary’ infection with one serotype, ‘secondary’ infections by one or more of the other serotypes can precipitate ‘antibody-dependant enhancement’ (ADE). Resolution of this issue is hampered by the absence of a reliable animal model. In addition, there is a lack of consensus regarding the validity of a graded set of criteria to categorise severity. Both these issues are of prime importance for the management and treatment of patients, and to the acceptance of dengue vaccines.
Epidemiology
- Dengue is endemic in more than 100 countries in Africa, the Americas, South and South-east Asia, and the Western Pacific region. ECDC monitors the current dengue transmission worldwide.
- Dengue viruses are highly mobile and transported by infected travellers. All four serotypes now co-circulate in many places around the world. The number of dengue cases has been increasing notably in the past few decades, and large outbreaks have been reported.
- Imported cases of dengue are frequently reported by travellers returning to the EU from endemic areas. This may generate a local transmission in areas where the vector is present. Since 2010, several autochthonous dengue outbreaks were reported in the EU.
- Prior to 2010, the last dengue epidemics in the European continent happened in Greece from 1927–28, with high mortality and Aedes aegypti as the mosquito vector.
- Through entomological surveillance, maps showing the distribution of potential dengue vectors in Europe are regularly updated. At the present time, the presence of Aedes aegypti in Madeira is a main concern.
- Enhanced surveillance of dengue in areas where potential vectors are present during the mosquito season is crucial for an early detection and appropriate vector and disease control measures.
- Early detection of infectious dengue patients is important to prevent local transmission in areas where the vector is present and active. Dengue is a notifiable disease in the EU and information is collected through The European Surveillance System (TESSy).
Transmission
- The incubation period of the dengue virus is 3–14 days, with an average of 4–7 days.
- Viraemia reaches high titres on the day before the onset of symptoms. It is generally high enough to infect mosquitoes for the next four days.
- Immunity to any of the four serotypes is probably life-long, but this does not confer protective immunity to the other three serotypes.
- Humans are the main amplifying host of the virus. In tropical and sub-tropical urban areas, the viruses are maintained in a human/mosquito cycle.
- Although bites from infected mosquitoes are the predominant mode of transmission, non-vectorial transmissions (e.g., mucocutaneous, nosocomial, sexual, intrapartum and perinatal transmission, as well as transmission through breastfeeding, laboratory accident, blood transfusion, bone marrow transplant and organ transplant) have also been reported.
- Mosquitoes acquire the virus when they feed on a viraemic host, after which the virus infects many tissues (in a susceptible species), including the salivary glands. The ‘extrinsic incubation period’ i.e. the time required for the mosquito to become infective, is about ten days at 27° C.
- New infections in humans can occur when saliva from mosquitoes containing virus is injected into a non-immune host i.e. humans, during subsequent blood meals.
- There is some evidence that forest monkeys are involved in a ‘jungle cycle’ with forest mosquitoes serving as vectors in south-eastern Asia and western Africa. However, there is no evidence to suggest that these viruses are responsible for large epidemics.
- The virus circulates between humans in rural and urban areas. Dengue is essentially a rural and urban disease because its principal vector, Aedes aegypti, is abundant in the peri-domestic environment. The species is a highly effective vector: it feeds almost exclusively on humans, breeds in small human-made objects that contain water, rests inside buildings, and is rarely found at a distance of more than 50 meters from human habitation. Its biting habits tend to be diurnal.
- A second species, the Asian tiger mosquito, Aedes albopictus, can also be common in the peri-domestic environment, particularly in urban areas with abundant vegetation. However, it is widely regarded as a ‘secondary’ vector because it is not host-specific. Blood meals are taken from animals that are not susceptible to the dengue virus, and therefore, do not participate in the transmission cycle. Nevertheless, epidemics have occurred in places where this mosquito was the only vector species present.
- Aedes aegypti was once present in Europe and responsible for large epidemics of yellow fever and dengue. Its disappearance from Europe after World War II has never been explained. Currently, it is present in Madeira, and it is conceivable that it could become re-established and widespread in Europe.
- The Aedes albopictus mosquito is present in southern Europe and well adapted to winter temperatures. It is likely to extend its range northwards. It is already a major nuisance in several Mediterranean countries, and has been responsible for autochthonous cases of dengue in southern Europe since 2010.
Diagnostics
- The dengue viral genome can be detected by reverse transcription polymerase chain reaction (RT-PCR) in blood specimens up to the fifth day of illness.
- Another approach is the detection of the non-structural protein 1 (NS1) dengue antigen up to the fourth day post-onset of symptoms. However, sensitivity of the assay depends on the serotype.
- Determination of the dengue serotype and genotype is important for epidemiological studies; co-circulation of different dengue serotypes during an outbreak is not uncommon.
- Viral isolation is done for research purposes.
- Serological diagnosis can be performed by the detection of dengue IgM antibodies in serum specimen from the fifth to sixth day of illness, or the detection of a four-fold rise of specific Immunoglobulin G (IgG) antibody titre on a pair of sera (acute and convalescent specimens).
- In a secondary dengue infection, dengue IgM antibodies usually appear earlier from the second to third day post-onset of symptoms, and with a shorter duration. An increase of dengue IgG titre has to be measured.
- Serological cross-reactions between dengue viruses and closely related flaviviruses have also been reported.
Case management and treatment
Supportive therapy is the only option to treat dengue, with strict avoidance of aspirin and other anticoagulants.
Public health control measures
- An integrated vector management programme aiming to reduce mosquito vector density in a sustainable manner is of primary importance. Intersectoral collaboration and efficient public communication strategies to ensure community participation are also required for a sustainable vector control programme.
- Activities supporting the reduction of mosquito breeding sites in outdoor/indoor areas by draining or discarding sources of standing water at the community level include:
— removal of all open containers with stagnant water in and surrounding houses on a regular basis (flower plates and pots, used tyres, tree-holes, and rock pools); or, if that is not possible, treatment with larvicides);
— tight coverage of water containers, barrels, wells, and water storage tanks;
— wide use of window/door screens by the population.
- Measures aiming to control larvae and adult mosquito vector populations can be applied in an outbreak situation.
- In affected outbreak areas, elimination of adult mosquitoes through aerial spraying with insecticides can be considered.
Infection control, personal protection and prevention
- Prevention is for the most part based on protection against mosquito bites. Aedes mosquitoes have diurnal biting activities in both indoor and outdoor environments. Therefore, personal protection measures should be applied all throughout the day, especially during the hours of the highest mosquito activity (mid-morning, late afternoon to twilight). Personal protective measures against mosquito bites include the use of mosquito bed nets (preferably insecticide-treated nets), sleeping or resting in screened or air-conditioned rooms, wearing clothes that cover most of the body, and using mosquito repellent in accordance with the instructions indicated on the product label.
- Travellers, especially children, pregnant women, and people with immune disorders or severe chronic illnesses, should consult their doctor or seek advice from a travel clinic to receive personalised recommendations on use of repellents and protection before travelling to dengue-endemic areas.
- Travellers should seek medical care if they present with symptoms compatible with dengue after returning from dengue-endemic areas.
- Irrespective of symptoms, travellers should protect themselves against mosquito bites for three weeks after returning from dengue-endemic areas to regions where Aedes albopictus and/or Aedes aegypti are present during the vector activity season (May–November).
- Two dengue vaccines have been granted an authorisation by the European Medicines Agency (EMA) for use in the EU: Dengvaxia (by Sanofi Pasteur) and Qdenga (by Takeda GmbH).
Dengvaxia was granted a marketing authorisation in the EU on 12 December 2018. It is indicated for the prevention of dengue disease in individuals aged 6–45 years, who have had a previous dengue virus infection. It is a tetravalent, live attenuated, recombinant dengue vaccine (CYD-TDV) with chimeric yellow fever-dengue virus construct that contains proteins from the four dengue virus serotypes. Dengvaxia is recommended to be administered in a three-doses schedule, six months apart, and must only be given to people who have had a positive test result showing a previous infection with dengue virus.
Qdenga was granted a marketing authorisation in the EU on 5 December 2022. It is indicated for the prevention of dengue disease in individuals from four years of age. It is a live attenuated vaccine that contains the four serotypes of dengue virus. It consists of an attenuated DENV-2 (DEN2-PDK-53), whereby three chimeric viruses containing the pre-membrane M and envelope proteins of DENV-1, DENV-3, and DENV-4 are inserted into the DENV2-backbone. The main difference to CYD-TDV (Dengvaxia), therefore, is the presence of non-structural proteins because of the DENV2-backbone. It is recommended to be administered in a two-dose schedule with an interval of three months between doses.
Updates on product information and authorisation details for use in the EU can be found on the EMA’s webpages: Dengvaxia (Dengvaxia | European Medicines Agency (EMA)) and Qdenga (Qdenga | European Medicines Agency (EMA)). Both vaccines should be used in accordance with official recommendations from international or national public health authorities.
References
- Gubler DJ. Dengue viruses: their evolution, history and emergence as a global public health problem. Wallingford: Oxon, UK; New York: CABI Books. CAB International; 1997. p. 478. Available at: https://www.cabidigitallibrary.org/doi/10.1079/9781845939649.0001
- La Ruche G, Souarès Y, Armengaud A, Peloux-Petiot F, Delaunay P, Desprès P, et al. First two autochthonous dengue virus infections in metropolitan France, September 2010. Euro Surveill. 2010 Sep 30;15(39):19676. Available at: https://www.eurosurveillance.org/content/10.2807/ese.15.39.19676-en
- Reiter P. Oviposition, dispersal, and survival in Aedes aegypti: implications for the efficacy of control strategies. Vector Borne Zoonotic Dis. 2007;7(2):261-73 . Available at: https://www.liebertpub.com/doi/10.1089/vbz.2006.0630
- Reiter P, Gubler DJ. Surveillance and control of urban dengue vectors. Dengue and dengue hemorrhagic fever. New York: CAB International 1997; p. 425–462. Available at: https://www.cabidigitallibrary.org/doi/10.1079/9781845939649.0481
- Reiter P. Yellow fever and dengue: a threat to Europe. Euro Surveill. 2010 Mar 11;15(10):pii=19509. Available at: https://www.eurosurveillance.org/content/10.2807/ese.15.10.19509-en
- Schmidt-Chanasit J, Haditsch M, Schoneberg I, Gunther S, Stark K, Frank C. Dengue virus infection in a traveller returning from Croatia to Germany. Euro Surveill. 2010 Oct 7;15(40):19677. Available at: https://www.eurosurveillance.org/content/10.2807/ese.15.40.19677-en
- Shepard DS , Coudeville L, Halasa YA, Zambrano B, Dayan GH. Economic impact of dengue illness in the Americas. Am J Trop Med Hyg. 2011 Feb; 84(2): 200–207. Available at: https://www.ajtmh.org/view/journals/tpmd/84/2/article-p200.xml
- Wilder-Smith A, Ooi EE, Vasudevan SG, Gubler DJ. Update on dengue: epidemiology, virus evolution, antiviral drugs, and vaccine development. Curr Infect Dis Rep. 2010 May;12(3):157-64. Available at: https://link.springer.com/article/10.1007/s11908-010-0102-7
- Wilder-Smith A. Risk of Dengue in Travelers: Implications for Dengue Vaccination. Curr Infect Dis Rep. 2018 Oct 29;20(12):50. Available at: https://link.springer.com/article/10.1007/s11908-018-0656-3
- European Medicines Agency (EMA). Dengvaxia EPAR Product Information. Amsterdam: EMA; 2022. Available at: https://www.ema.europa.eu/en/documents/product-information/dengvaxia-epar-product-information_en.pdf
- European Medicines Agency (EMA). Qdenga EPAR Product Information. Amsterdam: EMA; 2022. Available at: https://www.ema.europa.eu/en/documents/product-information/qdenga-epar-product-information_en.pdf
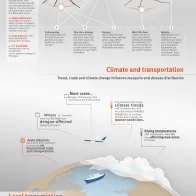
What are emerging/tropical mosquito-borne diseases? What are the different species of mosquitoes in Europe and the diseases they can carry?
