Disease information about malaria
Case definition
Malaria is a notifiable disease in the European Union (EU). The European case definition is available here.
The pathogen
Malaria in humans is an acute or subacute infectious disease caused by parasites of one of six species of the genus Plasmodium (Haemosporida: Plasmodiidae) of the phylum Apicomplexa: P. falciparum, P. vivax, P. ovale wallikeri, P. ovale curtisi, P. malariae, and P. knowlesi.
Clinical features and sequelae
Malaria is characterised by fever and influenza-like symptoms, including chills, headache, myalgia, and malaise; these symptoms (particularly fever) can occur at intervals in a pattern that varies by species. Malaria can be associated with anaemia and jaundice, and can cause kidney failure and an enlarged spleen. Infected red blood cells can clog small blood vessels in the brain, resulting in cerebral malaria, which is particularly common in P. falciparum infections, and can cause seizures, mental confusion, coma, and death. People who survive cerebral malaria may have neurological sequelae, cognitive deficits and behavioural alterations [1].
The clinical presentation of malaria very much depends on the level of immunity to malaria in the patient. While some immunity can be due to innate factors, in endemic areas immunity is mostly acquired through repeated exposure to Plasmodium. As a result, in highly endemic areas populations at higher risk of severe malaria are children aged under five years and pregnant women. Due to a tendency of Plasmodium-infected cells to accumulate in the placenta, malaria can also have negative effects on the growth and development of unborn children and can even cause infant death [2]. For people living in low endemic or epidemic-prone areas, and travellers from non-malaria regions, all ages are at risk of infection and severe disease.
Epidemiology
Malaria is a major global public health issue: it is endemic in over 80 countries, and causes around 250 million infections and 600 000 deaths annually worldwide [3].
Infections with P. falciparum and P. vivax represent the major part of the global burden of malaria. Plasmodium falciparum is the most prevalent malaria parasite in West Africa (almost 100%), Central Africa (100%), high transmission countries in East and Southern Africa (almost 100%), low transmission countries in East and Southern Africa (about 90%), the Eastern Mediterranean region (about 70%), the Western Pacific (about 70%), and South-East Asia (about 50%), while P. vivax is the dominant malaria species in the Americas (about 70%) [3].
During the 20th century, malaria was eradicated from many temperate areas, including the whole of Europe. With global climate change, there is the potential for the reappearance of malaria in countries where it was previously eradicated, but this is relatively small where functioning health systems are able to detect and treat the disease before it spreads. Mosquitoes that can transmit malaria are still present in temperate areas, including in Europe.
Nearly all malaria cases reported by EU/EEA countries are imported, and as such, malaria in Europe is mainly a travel medicine issue. Seasonality and age distribution of cases in Europe most likely reflect travel patterns to malaria-endemic countries [4]. The European countries that report the highest numbers of imported cases have historical, economic, linguistic, and cultural links with endemic areas, particularly in Africa and the Americas. Most of the imported malaria cases in France are linked to travel routes from West Africa [5]. A substantial proportion of imported malaria cases in the EU/EEA occur among people who recently emigrated from malaria-endemic countries and migrants who have travelled to visit friends and relatives in malaria-endemic countries [6,7]. The EU Outermost Region French Guiana is endemic for malaria [8].
A few autochthonous malaria cases are reported in Europe annually. ‘Introduced cases’, which are first-generation infections in a geographic area transmitted by local mosquitoes infected by imported malaria cases (mainly P. vivax), have been detected in the EU/EEA since 2009 [9]. Other autochthonous cases might have resulted from healthcare-associated infections [10] or, more rarely, from congenital infections [11,12].
Historically, the most important vectors of malaria in Europe were Anopheles atroparvus, Anopheles labranchiae and Anopheles sacharovi (all three members of the Anopheles maculipennis species complex) and Anopheles plumbeus. Although rare, Plasmodium transmission via infectious mosquitoes imported from endemic areas – termed ‘airport malaria’ when in the vicinity of international airports and ‘luggage malaria’ when infected mosquitoes have been suspected to have travelled in luggage – sporadically occurs [13].
Transmission
The incubation period from infection to the first symptoms varies between one and four weeks in most cases. Depending on the Plasmodium species involved, much longer incubation periods are possible. Due to the occurrence of dormant stages, a single infection event of P. vivax or P. ovale can be responsible for a series of ‘relapses’ that can be months or years apart if the disease is not treated properly.
People become infectious to mosquitoes only after the formation of gametocytes (see ‘Parasite life cycle’, below), which typically occurs during the second week after the onset of parasitaemia in P. falciparum infections [14]. Infected humans remain infectious to mosquitoes as long as they carry mature sexual forms of Plasmodium. This period depends on the Plasmodium species, on the immune status of the patients, and on treatment provided; in endemic areas it generally lasts for several weeks. However, asymptomatic P. falciparum infections can persist for up to a decade or longer [15].
For all Plasmodium species known to infect humans, the main mode of transmission is by the bite of infected female Anopheles mosquitoes. About 60 to 100 anopheline species in the world are able to transmit malaria. There is no animal reservoir for P. falciparum, P. vivax, P. ovale, or P. malariae. Macaques are the animal reservoir of P. knowlesi.
Occasionally, transmission can occur by blood transfusion [16], organ transplantation [17], needle-sharing, or congenitally from mother to foetus [18].
Parasite life cycle
During an infective mosquito bite, malaria sporozoites are excreted by the salivary gland of the (female) mosquito and are transported by the bloodstream to the liver within minutes. The sporozoites invade liver cells and become schizonts.
During the schizogony stage, which takes about six to 15 days, depending on the Plasmodium species, there are multiple rounds of nuclear division, after which the schizont segments into merozoites which are released into the bloodstream.
A characteristic of P. vivax and P. ovale is that some of the sporozoites do not immediately begin to grow and divide after entering a hepatocyte, but can remain in a dormant, hypnozoite stage for weeks, months, or even years. The merozoites infect red blood cells and transform into trophozoites, the feeding stage. After growth, most trophozoites develop into new merozoites. These merozoites burst out of the red blood cells and invade others. This rupturing of the membranes of the parasitised blood cells is associated with fever in the host.
Some trophozoites do not develop into merozoites but develop into sexually differentiated stages which can infect mosquitoes. These sexual stages take approximately eight to 10 days to reach full maturity.
When ingested by a mosquito feeding on an infected host, in the gut of the mosquito, the male and female sexual stages fuse into ookinetes which cross the midgut wall and form oocysts. The oocyst then matures to form multiple haploid sporozoites. The rate of maturation is temperature-dependent, but typically takes one to three weeks. The immature sporozoites break through the oocyst wall and migrate to the mosquito’s salivary glands, where they mature and can infect another human during the next bite of the mosquito.
Diagnostics
The gold standard for laboratory confirmation of malaria remains the identification of malaria parasites through microscopy of a blood sample. Alternative methods for laboratory diagnosis include: 1) antigen detection using rapid diagnostic tests, a useful alternative in situations where reliable microscopic diagnosis is not available; 2) molecular diagnosis through Polymerase Chain Reaction (PCR) or Loop-mediated Isothermal Amplification (LAMP), which is more accurate than microscopy; and 3) serology, using indirect immuno-fluorescence assay (IFA) or enzyme-linked immuno-sorbent assay (ELISA). Serology does not detect current infections but rather measures past malaria experience.
Case management and treatment
Although malaria can be fatal, illness and death from it are largely preventable. Anti-malarial treatment policies vary between countries, and depend on the epidemiology of the disease, transmission, patterns of drug resistance, and political and economic contexts. There is no universal treatment scheme. The drugs currently available for malaria treatment include chloroquine, amodiaquine, primaquine sulfadoxine-pyrimethamine, mefloquine, atovaquone-proguanil, quinine, doxycycline, and artemisinin derivatives often used in combination therapy.
Public health prevention and control measures (for public health authorities)
There is a need for continuous malaria surveillance, preparedness, and prevention. Clinicians’ awareness about malaria in travellers should remain a focus of attention, as the main risk of malaria in the EU/EEA is for travellers to malaria-endemic countries (see section ‘Advice to travellers’). Early diagnosis and prompt treatment of imported and introduced cases are the basic elements of malaria control in the EU/EEA, including active case finding.
Although the probability of becoming infected with Plasmodium parasites through an infectious mosquito bite is extremely low in Europe, personal protective measures against mosquito bites are recommended in general to prevent mosquito-borne diseases during times when mosquitoes are active.
In malaria-endemic countries, malaria is controlled through a combination of vector control (mainly through the distribution of insecticide-treated nets and indoor residual spraying with insecticides), preventive chemotherapies (such as intermittent preventive treatment of malaria in pregnancy, seasonal or perennial chemoprevention) and vaccines (recommended by the World Health Organization for children living in areas with moderate to high transmission), and case management by testing for and treating malaria [19].
Infection control, personal protection and prevention (for the health facilities)
Vigilance should remain high regarding malaria transmission through substances of human origin (e.g. blood products or organ transplants). Healthcare providers should be aware that healthcare-associated transmission of malaria is possible irrespective of the Plasmodium species involved. Clinicians should therefore consider the possibility of healthcare-associated malaria in hospitalised or recently discharged patients who develop an unexplained fever or malaria-like clinical syndrome, especially if their hospital admission coincided with that of another patient admitted with malaria [10].
Advice to travellers
Travellers to malaria-endemic areas should be aware of the risks of becoming infected with Plasmodium. Individuals visiting friends and relatives in malaria-endemic countries are less likely than other travellers to seek pre-travel advice and use the recommended malaria prevention measures. In addition, the duration of their trips tends to be longer, with increased exposure as a result [20].
Because of the nocturnal feeding habits of most Anopheles mosquitoes, malaria transmission primarily occurs at night. Personal protective measures to reduce the risk of mosquito bites include the use of mosquito bed nets (preferably insecticide-treated nets), sleeping or resting in screened or air-conditioned rooms, the wearing of clothes that cover most of the body, and the use of mosquito repellent in accordance with the instructions indicated on the product label.
Malaria chemoprophylaxis is recommended for European travellers to malaria-endemic countries. Malaria was by far the most frequently diagnosed arthropod-borne disease among travellers arriving from Africa to Europe, despite the existence of chemoprophylaxis [21]. The choice of drugs depends on the travel destination, the duration of potential exposure to vectors, parasite resistance pattern, level and seasonality of transmission, age, and pregnancy status (see WHO’s requirements and recommendations for international travellers, including a list of affected countries [22]).
References
- Rosa-Goncalves P, de Sousa LP, Maia AB, Ribeiro-Gomes FL, Gress C, Werneck GL, et al. Dynamics and immunomodulation of cognitive deficits and behavioral changes in non-severe experimental malaria. Front Immunol. 2022;13:1021211. Available at: https://www.ncbi.nlm.nih.gov/pubmed/36505414
- Zakama AK, Ozarslan N, Gaw SL. Placental Malaria. Curr Trop Med Rep. 2020;7(4):162-71. Available at: https://www.ncbi.nlm.nih.gov/pubmed/32953387
- World Health Organization (WHO). World malaria report 2022. Geneva: 2022 WHOAvailable at: https://www.who.int/teams/global-malaria-programme/reports/world-malaria-report-2022
- European Centre for Disease Prevention and Control. Travel-associated malaria cases: place of infection for cases imported to the European Union/European Economic Area. 2024. Available at: https://www.ecdc.europa.eu/en/infectious-disease-topics/malaria/surveillance-and-disease-data/travel-associated-malaria-cases
- Tatem AJ, Jia P, Ordanovich D, Falkner M, Huang Z, Howes R, et al. The geography of imported malaria to non-endemic countries: a meta-analysis of nationally reported statistics. Lancet Infect Dis. 2017 Jan;17(1):98-107. Available at: https://www.ncbi.nlm.nih.gov/pubmed/27777030
- European Centre for Disease Prevention and Control (ECDC). Assessing the burden of key infectious diseases affecting migrant populations in the EU/EEA. Stockholm: ECDC 2014. Available at: https://www.ecdc.europa.eu/en/publications-data/assessing-burden-key-in…
- Grobusch MP, Weld L, Goorhuis A, Hamer DH, Schunk M, Jordan S, et al. Travel-related infections presenting in Europe: A 20-year analysis of EuroTravNet surveillance data. Lancet Reg Health Eur. 2021 Feb;1:100001. Available at: https://www.ncbi.nlm.nih.gov/pubmed/35081179
- Musset L, Pelleau S, Girod R, Ardillon V, Carvalho L, Dusfour I, et al. Malaria on the Guiana Shield: a review of the situation in French Guiana. Mem Inst Oswaldo Cruz. 2014 Aug;109(5):525-33. Available at: https://www.ncbi.nlm.nih.gov/pubmed/25184998
- National Public Health Organization (NPHO). Annual epidemiological surveillance report Malaria in Greece, 2023.
- European Centre for Disease Prevention and Control (ECDC). Rapid Risk Assessment: Hospital-acquired malaria infections in the European Union. Stockholm: ECDC; 2018. Available at: https://ecdc.europa.eu/sites/portal/files/documents/2018-04-30-RRA-Hospital-acquired-Malaria-European-Union-with%20erratum-1.pdf
- European Centre for Disease Prevention and Control (ECDC). Malaria Annual Epidemiological Report for 2014. Stockholm: ECDC 2016. Available at: https://www.ecdc.europa.eu/en/publications-data/malaria-annual-epidemio…
- Guida Marascia F, Colomba C, Abbott M, Gizzi A, Anastasia A, Pipito L, et al. Imported malaria in pregnancy in Europe: A systematic review of the literature of the last 25 years. Travel Med Infect Dis. 2023 Nov-Dec;56:102673. Available at: https://www.ncbi.nlm.nih.gov/pubmed/38008239
- Hallmaier-Wacker LK, van Eick MD, Briët O, Delamare H, Falkenhorst G, Houze S, et al. Airport and luggage (Odyssean) malaria in Europe: a systematic review. Euro Surveill. 2024 Oct;29(41); Available at: https://www.eurosurveillance.org/content/10.2807/1560-7917.ES.2024.29.41.2400237
- Harinasuta T, Bunnang D. The clinical features of malaria. In: Wernsdorfer WH, McGregor I, editors. Malaria: principles and practice of malariology. London: Churchill Livingstone; 1988.
- Ashley EA, White NJ. The duration of Plasmodium falciparum infections. Malar J. 2014 Dec 16;13:500. Available at: https://www.ncbi.nlm.nih.gov/pubmed/25515943
- Ahmadpour E, Foroutan-Rad M, Majidiani H, Moghaddam SM, Hatam-Nahavandi K, Hosseini SA, et al. Transfusion-Transmitted Malaria: A Systematic Review and Meta-analysis. Open Forum Infect Dis. 2019 Jul;6(7):ofz283. Available at: https://www.ncbi.nlm.nih.gov/pubmed/31334300
- Fabiani S, Fortunato S, Bruschi F. Solid Organ Transplant and Parasitic Diseases: A Review of the Clinical Cases in the Last Two Decades. Pathogens. 2018 Jul 31;7(3). Available at: https://www.ncbi.nlm.nih.gov/pubmed/30065220
- Bilal JA, Malik EE, Al-Nafeesah A, Adam I. Global prevalence of congenital malaria: A systematic review and meta-analysis. Eur J Obstet Gynecol Reprod Biol. 2020 Sep;252:534-42. Available at: https://www.ncbi.nlm.nih.gov/pubmed/32620512
- World Health Organization (WHO). WHO guidelines for malaria 2023 Contract No.: WHO/UCN/GMP/2023.01 Rev. 1.
- Center for Disease Control and Prevention (CDC). Recommendations for Immigrants from Malaria-Endemic Countries Planning to Return "Home" to Visit Friends and Relatives. Atlanta: CDC; 2018.
- Gossner CM, Hallmaier-Wacker L, Briet O, Haussig JM, de Valk H, Wijermans A, et al. Arthropod-borne diseases among travellers arriving in Europe from Africa, 2015 to 2019. Euro Surveill. 2023 Feb;28(7) Available at: https://www.ncbi.nlm.nih.gov/pubmed/36795503
- World Health Organization (WHO). International travel and health – 18 November 2022 – Country list – Vaccination requirements and recommendations for international travellers; and malaria situation per country. Geneva: WHO; 2022. Available at: https://www.who.int/publications/m/item/vaccination-requirements-and-recommendations-for-international-travellers-and-malaria-situation-per-country-2022-edition
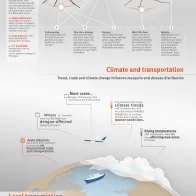
What are emerging/tropical mosquito-borne diseases? What are the different species of mosquitoes in Europe and the diseases they can carry?

This species is a known persistent biter of humans. It is suspected of having contributed to malaria transmission in the past and has been shown to be a competent vector of both tropical and Eurasian strains of malaria.

Remains widespread in Europe, mostly coastal but also found in freshwater habitats. Implicated as a key vector of malaria during the twentieth century.

Anopheles labranchiae is reportedly an endophilic species which will aggressively attack human hosts.

Anopheles sacharovi is an important vector of malaria throughout its distribution
The Annual Epidemiological Reports (AERs) are a key ECDC publication on the epidemiology of communicable diseases of public health significance in Europe.
