Malaria - Annual Epidemiological Report 2016 [2014 data]
Malaria Annual Epidemiological Report for 2014
English (162.73 KB - PDF)Malaria, surveillance systems overview, 2014
English (24.3 KB - XLSX)Key facts
- 6 017 confirmed malaria cases were reported to TESSy in 2014.
- The notification rate in 2014 was 1.24 cases per 100 000 population.
- 99.9% of cases for which travel information was provided were travel related. Five cases were locally acquired (three reported by Spain and two by France).
- The highest notification rates were reported in males in age groups 15–24 and 25–44 years.
- The number of cases increased during the summer months, and a smaller upsurge was observed in January. This reflects most probably travel patterns.
- The worldwide decrease in malaria incidence did not yet result in a decrease of travel-related cases reported in the EU/EEA. Therefore, awareness among travellers and clinicians, particularly among those visiting friends and relatives in endemic countries, should be maintained.
- Local transmission of Plasmodium vivax remains possible in the EU and stresses the need for continued surveillance, preparedness and prevention.
Methods
Click here for a detailed description of the methods used to produce this annual report
- 26 EU/EEA countries provided information on malaria. No data were reported by Denmark, Germany, Iceland, Italy and Liechtenstein.
- 23 countries used the EU case definition, two countries (Belgium and Finland) did not specify which case definition was used, and one country used an alternative case definition (France). Surveillance is mostly case based except in Bulgaria and Croatia. The surveillance coverage for France is not nationwide.
- All reporting countries have a comprehensive surveillance system. Reporting is compulsory in 23 countries, voluntary in two countries (Belgium and France), and not specified in the United Kingdom. Disease surveillance is mostly passive except in Belgium, the Czech Republic, Slovakia and the United Kingdom, where active surveillance is in place. Greece also has active disease surveillance in high-risk areas. (Annex 1).
Epidemiology
Most reported malaria cases were travel related. Five cases were reported as locally acquired: two in France and three in Spain. The Spanish malaria cases were characterised as follows:
- One case of congenital Plasmodium falciparum malaria. A newborn whose mother had recently returned from Equatorial Guinea was diagnosed with malaria one week after birth. The baby had no symptoms but the laboratory tests identified P. falciparum.
- Induced infection: Plasmodium malariae in a patient who had received a kidney transplant. The donor had travelled to Equatorial Guinea. An antigenic study and a smear test were carried out before the transplant; both were negative. Two transplant recipients from the same donor did not develop symptoms, also with negative laboratory tests results. Both patients received preventive malaria treatment.
- Introduced infection: a Plasmodium vivax case. The patient had no history of travel or hospitalisation but lived a few kilometres from a town with a travel-related case. Molecular typing showed that the same strain of P. vivax was responsible for both infections. No infected mosquitoes were found during the entomological investigation.
The two locally acquired cases in France should be interpreted with caution: according to the French case definition, malaria cases are classified by default as locally acquired unless patients report that they travelled to malaria-endemic areas in the previous 12 months. The two patients did not report any recent travel but the investigation could not be completed because both patients were undocumented residents.
Greece recorded zero locally acquired cases in 2014, compared with three cases in 2013 and 20 cases in 2012.
The overall confirmed case rate in 2014 was 1.24 cases per 100 000 population, which is the highest rate observed during the period 2010–2014. The individual country rates varied between 0.05 cases (Poland) and 3.67 cases (Sweden) per 100 000 population. The rates in Sweden and Norway were notably higher than in previous years. In Sweden, the notification rate in 2014 was 3.67 cases (2013: 1.25 cases per 100 000 population), while in Norway the 2014 rate was 2.35 cases per 100 000 population (2013: 1.43 cases).
The highest number of confirmed cases notified in 2014 was observed in France (n=2 299), followed by the United Kingdom (n=1 510) (Table 1).
Age and gender distribution
In 2014, the overall rate of confirmed malaria cases was higher among men than women (1.75 cases and 0.74 cases per 100 000 population, respectively), and the male-to-female ratio was 2.4:1. The highest notification rate for males was in the 25–44-year-old age group (2.73 cases per 100 000 population), followed by the group of 15–24-year-olds (2.68 cases per 100 000 population).
Among females, the highest notification rate was in the age groups 15–24 years old and 25–44 years old (1.22 cases per 100 000 and 1.10 cases per 100 000 population, respectively) (Figure 2).
Seasonality
A marked seasonal trend was observed across all countries, with cases increasing during the summer holiday months (July–September) and a lower increase in January.
Trend
In the period 2010–2014 the highest number of reported cases was seen in 2014, but overall the trend appears to be stable.
Discussion
The confirmed notification rate of malaria reported by EU and EEA countries has remained stable over the last few years and hovers at about 100 000 population per year, with a slight increase in 2014 (1.24 cases per 100 000 population) compared with 2010–2013.
WHO reported that between 2000 and 2015, the rate of new cases of malaria worldwide fell by 37%. Malaria mortality rates decreased by 60% among all age groups globally, and an estimated 6.2 million malaria deaths have been averted globally since 2000 [1]. Current malaria control interventions seem to have considerably reduced the malaria incidence in Africa and outside Africa [2, 3]. The reduction in global malaria incidence did not yet result in a decline of the notification rate observed in the EU/EEA.
Nearly all (99.9%) of the reported malaria cases were imported and notified by EU and EEA countries that have strong ties with endemic areas (e.g. France and its French overseas territories). Seasonality and age distribution most likely reflect travel patterns to malaria-endemic countries. Information on the reasons for travel, i.e. holidays, visiting friends and relatives, or business, was not available. Travellers visiting friends and relatives in endemic countries constitute a significant group for malaria importation to the EU [4]. A review of the literature suggests that a substantial proportion of imported malaria cases in the EU/EEA occur among recent immigrants from malaria-endemic countries and among more settled migrants and their families who have travelled to visit friends and relatives in malaria-endemic home countries [5]. Outside continental Europe, some European territories are endemic for malaria (e.g. Mayotte and French Guiana); data for these regions are not collected through TESSy.
A small number of autochthonous transmission of malaria was reported over the last 10 years [6-9]. In 2014, one case of locally acquired Plasmodium vivax malaria was reported from Spain. In 2014, for the first time since 2009, Greece did not report any locally acquired cases. In 2015, however, Greece reported six locally acquired Plasmodium vivaxmalaria cases. One case each was reported from Farkadona–Trikala regional unit, Evrotas–Lakonia regional unit, Tempi–Larisa regional unit, Thiva–Viotia regional unit; two cases were notified in Marathon–East Attica regional unit [10].
Public health conclusions
The worldwide decrease in malaria incidence did not yet result in a decrease of the travel related malaria cases reported in the EU/EEA. Therefore, awareness among clinicians and travellers, particularly among those visiting friends and relatives in endemic countries, should be maintained high. Vigilance remains needed regarding transmission through substances of human origin (SoHO) e.g. blood products or organ transplant.
The data also indicate that local transmission of Plasmodium vivax remains possible in the EU, though the transmission route is not always easily detected. This emphasises the need for surveillance, preparedness and prevention in the EU/EEA. Further steps should be taken to improve the access to healthcare for migrants.
References
- World Health Organization. Malaria. Fact sheet: WHO/UNICEF report ‘Achieving the malaria MDG target’. 2015 [cited 2015 01 December 2015].
- Bhatt S, Weiss DJ, Cameron E, Bisanzio D, Mappin B, Dalrymple U, et al. The effect of malaria control on Plasmodium falciparum in Africa between 2000 and 2015. Nature, 2015. 526(7572): p. 207-211.
- Murray CJ, Ortblad KF, Guinovart C, Lim SS, Wolock TM, Roberts DA, et al. Global, regional, and national incidence and mortality for HIV, tuberculosis, and malaria during 1990–2013: a systematic analysis for the Global Burden of Disease Study 2013. Lancet, 2014. 384(9947): p. 1005-1070.
- Behrens RH, Neave PE, Jones CO. Imported malaria among people who travel to visit friends and relatives: is current UK policy effective or does it need a strategic change? Malar J. 2015 Apr 9;14:149.
- European Centre for Disease Prevention and Control. Assessing the burden of key infectious diseases affecting migrant populations in the EU/EEA. Stockholm: ECDC; 2014.
- Romi R, Boccolini D, Menegon M, Rezza G. Probable autochthonous introduced malaria cases in Italy in 2009–2011 and the risk of local vector-borne transmission. Euro Surveill. 2012 Nov 29;17(48).
- Arends JE1, Oosterheert JJ, Kraaij-Dirkzwager MM, Kaan JA, Fanoy EB, Haas PJ, et al. Two cases of Plasmodium falciparum malaria in the Netherlands without recent travel to a malaria-endemic country. Am J Trop Med Hyg. 2013 Sep;89(3):527-30 .
- Gallien S1, Taieb F, Hamane S, De Castro N, Molina JM. Autochthonous falciparum malaria possibly transmitted by luggage-carried vector in Paris, France, February 2013. Euro Surveill. 2013 Oct 3;18(40).
- Odolini S, Gautret P, Parola P. Epidemiology of imported malaria in the Mediterranean region. Mediterr J Hematol Infect Dis. 2012;4(1):e2012031 .
- Hellenic Center for Disease Control and Prevention. Epidemiological surveillance report, malaria in Greece, 2015, up to 16/10/2015. Hellenic Center for Disease Control and Prevention: Athens; 2015.
_________
* The European Surveillance System (TESSy) is a system for the collection, analysis and dissemination of data on communicable diseases. EU Member States and EEA countries contribute to the system by uploading their infectious disease surveillance data at regular intervals.
Reported malaria cases: number and rate per 100 000 population, EU/EEA, 2010–2014

Number of reported and confirmed malaria cases, EU/EEA, 2014
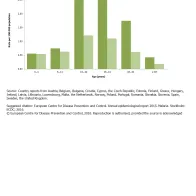
Confirmed malaria cases, by age and gender, EU/EEA, 2014
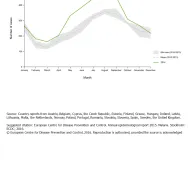
Seasonal distribution of confirmed malaria cases, EU/EEA, 2014 compared with 2010−2013
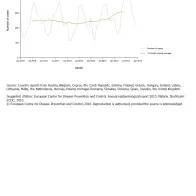
Trend and number of confirmed malaria cases, EU/EEA, 2010−2014
Share this page
