Chikungunya - Annual Epidemiological Report 2016 [2014 data]
Chikungunya - Annual Epidemiological Report 2016 [2014 data]
English (157.09 KB - PDF)Chikungunya, surveillance systems overview, 2014
English (23.85 KB - XLSX)Key facts
- 1 461 cases were reported in TESSy in 2014; 875 of these cases were confirmed.
- Eleven (0.8%) cases were locally acquired in France, 1 406 were travel related, and the status of 44 cases was unknown.
- The EU/EEA notification rate in 2014 was 0.31 cases per 100 000 population.
- There was a 20-fold increase in the number of cases in 2014 compared with 2013 (72 cases), mainly due to travel-associated cases from the Caribbean and the Americas, where a large outbreak started in 2013.
- In October 2014, an outbreak of 11 confirmed autochthonous chikungunya cases was detected in Montpellier, France. This was the first outbreak of chikungunya fever in Europe since the 2007 Italian epidemic.
- The highest rates were reported in females; the age groups 25–44 years and 15–24 years had the highest rates for both genders.
- The number of cases increased during the summer holiday months and stayed relatively high during the second half of the year.
Methods
Click here for a detailed description of the methods used to produce this annual report
• Of the 23 EU/EEA countries that reported chikungunya cases to TESSy, 10 reported zero cases. No data were available from Austria, Bulgaria, Cyprus, Denmark, Iceland, Liechtenstein, Norway and Portugal.
• Data for chikungunya fever reported within the EU/EEA are very heterogeneous as no specific case definition for chikungunya is available yet. Sixteen countries used the generic EU case definition for all viral haemorrhagic fevers, three countries did not specify which case definition was used (Belgium, Finland and France), and four countries used a different case definition (Czech Republic, Germany, Italy and the United Kingdom).
• Most reporting countries have a comprehensive surveillance system; the Netherlands uses a different type of system; no information was available from Sweden.
• Twenty countries reported having a compulsory notification system, whereas Belgium and the United Kingdom reported having a voluntary system. Sweden did not report this information.
• Disease surveillance for chikungunya is mostly passive except in the Czech Republic, Slovakia and the United Kingdom, where active systems are in place. The type of system is not specified in Sweden (Annex 1). Data reporting is case based and at the national level, with the Netherlands being the only exception.
Epidemiology
Most chikungunya fever cases were travel related (n=1406), 11 cases – all reported by France – were locally acquired, and for 44 cases the place of infection was unknown.
The 1 461 cases reported in 2014 represented a 20-fold increase compared with 2013. This was the highest number of cases reported for a single year since the start of reporting to TESSY in 2008 (Figure 4). The majority of cases was in people aged 25–44 years and 45–64 years. Most of the cases were reported as occurring during the summer months, but case numbers also remained high during the second half of the year.
The notification rate in 2014 (0.31 cases per 100 000 population) was much higher than in 2013 (0.02 per 100 000 population) and in previous years (Table 1).
The highest number of cases was reported in France (550), followed by the United Kingdom (301) and Spain (272), probably reflecting the travelling patterns to destinations with chikungunya outbreaks in 2014 (Figure 1).
Age and gender distribution
Overall, 59.1% of cases were females with a notification rate of 0.37 per 100 000 compared with 0.26 per 100 000 in males; the male-to-female ratio was 0.7:1. The highest notification rate of chikungunya fever was observed in the 25–44- and 45–64-year-old age groups (0.43 and 0.45 per 100 000 population, respectively). In both age groups the rate was higher among females (0.54 and 0.53 cases per 100 000 population) than among males (0.32 and 0.35 cases per 100 000 population) (Figure 2). This pattern was also seen in 2013, although less pronounced.
Seasonality
Reporting of chikungunya cases sharply increased in April, peaking in June (n=225) and July (n=228), followed by a slow decrease. During the second half of the year the number of reported cases stayed relatively high, due to ongoing outbreaks in the Americas. Before 2014 (2010–2013) no clear seasonality could be detected for chikungunya in EU/EEA countries (Figure 3).
Enhanced surveillance in 2014
In 2014, importation status was available for 1 417 cases. Eleven of these cases (0.8 %) – all from France – were reported as locally acquired.
Among the travel-related cases that had information on probable country of infection (n=1 227), most were reported as being acquired in the Americas and the Caribbean (n=1 152; 94%). The distribution of cases reported as being acquired in the Caribbean is as follows: Dominican Republic (n=256, 21%), Guadeloupe (n=247, 20%), Martinique (n=170, 14%), Jamaica (n=105, 9%), Haiti (n=57, 5%) and French Guiana (n=50, 4%).
Among reported cases from 2013 with information on probable country of infection (n=59), most were acquired in the Philippines (n=16), India (n=15) and Indonesia (n=10).
Discussion
The number of reported chikungunya cases in the EU/EEA was markedly higher in 2014 compared with previous years. Higher case numbers can be linked to an ongoing outbreak in the Caribbean which resulted in a higher number of cases due to travel exposure.
Locally acquired cases of chikungunya were suspected in November 2013 and laboratory-confirmed in December 2013 in the Caribbean island of Saint Martin [1]. This was the first documented autochthonous transmission of chikungunya virus in the Caribbean. Chikungunya virus (Asian genotype) rapidly spread to the surrounding islands and reached, for the first time, South, Central and North America [2]. The Pan American Health Organization (PAHO) registered 1 118 678 cases in the Americas up to the end of 2014 (incidence rate 116 per 100,000 inhabitants). As of 20 November 2015, 596 893 cases were reported to PAHO [3]. Outbreaks were also reported in the Pacific region [4]. As a result of this widespread outbreak in the Americas, EU/EEA countries reported a 20-time increase in the total number of imported chikungunya cases in the EU in 2014 compared with the previous year (61 cases with information on probable country of infection in 2013).
The first identified outbreak of chikungunya fever in a temperate climate in 2007 in north-east Italy demonstrated the potential of the Aedes albopictus mosquito to transmit the virus at EU latitudes [5]. In 2010, indigenous transmission was reported for the second time in Europe, with the first two indigenous cases identified through enhanced surveillance in metropolitan France [6]. In 2011 and 2012, only imported cases of chikungunya were reported from EU and EEA countries.
In October 2014, an outbreak of 11 confirmed autochthonous chikungunya cases was detected in a district of Montpellier, a town in the south of France, which had been colonised by the vector Aedes albopictus since 2010. The primary case was a local resident who returned from Cameroon with an infection caused by a chikungunya virus of the East/Central/South African (ECSA) strain [7,8]. This was the first outbreak of chikungunya in Europe since the 2007 Italian epidemic. This new episode highlights the risk of locally acquired cases occurring in countries where competent Aedes mosquito vectors are established and where conditions are suitable for transmission, like in many Mediterranean countries of the EU [9].
Public health conclusions
Vigilance regarding imported cases of chikungunya and other diseases transmitted by Aedes mosquitoes and awareness among clinicians and travel clinic specialists should be raised in the EU, especially in areas where competent mosquito vectors are present and environmental conditions are suitable for transmission [9].
Preparedness plans to contain and/or mitigate the spread of chikungunya in the EU should include:
- Strengthening of surveillance systems, including the adoption of a specific case definition and the rapid detection and notification of cases at local, national and international levels
- Regular reviews of contingency plans for mosquito-borne outbreaks
- Education and engagement of the general public in the control of mosquito breeding sites
- Strengthening vector surveillance systems and rapid implementation of vector control measures around each case
- Considering the adoption of blood safety measures in affected areas; measures should be aligned with the ones for West Nile virus infection.
References
- Cassadou S, Boucau S, Petit-Sinturel M, Huc P, Leparc-Goffart I, Ledrans M. Emergence of chikungunya fever on the French side of Saint Martin island, October to December 2013. Euro Surveill. 2014;19(13).
- Van Bortel W, Dorleans F, Rosine J, Blateau A, Rousset D, Matheus S, et al. Chikungunya outbreak in the Caribbean region, December 2013 to March 2014, and the significance for Europe. Euro Surveill. 2014;19(13).
- Regional Office for the Americas of the World Health Organization. Chikungunya: statistic [sic] data [Internet]. Washington: World Health Organization; 2015 [cited 2015 Nov 26]. Available from: http://www.paho.org/hq/index.php?option=com_topics&view=readall&cid=5927&Itemid=40931&lang=en
- Nhan TX, Musso D. The burden of chikungunya in the Pacific. Clin Microbiol Infect. 2015 Jun;21(6):e47-8.
- Rezza G, Nicoletti L, Angelini R, Romi R, Finarelli AC, Panning M, et al. Infection with chikungunya virus in Italy: an outbreak in a temperate region. Lancet. 2007 Dec 1;370(9602):1840-6.
- Grandadam M, Caro V, Plumet S, Thiberge JM, Souares Y, Failloux AB, et al. Chikungunya virus, southeastern France. Emerg Infect Dis. 2011 May;17(5):910-3.
- Delisle E, Rousseau C, Broche B, Leparc-Goffart I, L'Ambert G, Cochet A, et al. Chikungunya outbreak in Montpellier, France, September to October 2014. Euro Surveill. 2015;20(17).
- Septfons A, Noël H, Leparc-Goffart I, Giron S, Delisle E, Chappert JL, et al. Surveillance du chikungunya et de la dengue en France métropolitaine. Bull Epidémiol Hebd. 2015;13-14:204-11.
- European Centre for Disease Prevention and Control. Mosquito maps [Internet]. 2015 [cited 2015 Oct 1].
_________
* The European Surveillance System (TESSy) is a system for the collection, analysis and dissemination of data on communicable diseases. EU Member States and EEA countries contribute to the system by uploading their infectious disease surveillance data at regular intervals.
Table 1. Reported chikungunya fever cases: number and rate per 100 000 population, EU/EEA, 2010–2014
Reported chikungunya fever cases: number and rate per 100 000 population, EU/EEA, 2010–2014
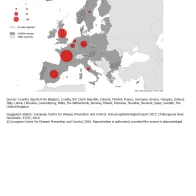
Number of reported chikungunya cases, EU/EEA, 2014
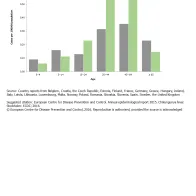
Reported chikungunya cases, by age and gender, EU/EEA, 2014
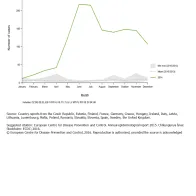
Seasonal distribution of reported chikungunya cases, EU/EEA, 2014 compared with 2010−2013 (minimum–maximum)

Trend and number of reported chikungunya cases, EU/EEA, 2010−2014
Share this page
