Typhoid and paratyphoid fever - Annual Epidemiological Report, 2016 [2014 data]
Typhoid and paratyphoid fever - Annual Epidemiological Report 2016
English (138.44 KB - PDF)Table. Typhoid, surveillance systems overview, 2016
English (24.41 KB - XLSX)Key facts
- Typhoid and paratyphoid fever are relatively rare diseases in the EU/EEA, mainly acquired while travelling to countries outside of the EU/EEA, particularly South Asia.
- In 2014, 934 confirmed cases were reported in 27 EU/EEA countries with an EU/EEA notification rate of 0.31 cases per 100 000.
- A decreasing trend of typhoid/paratyphoid fever has been observed in the EU/EEA in the last five years
- Typhoid fever is still more often reported than paratyphoid fever, although two vaccines are available against typhoid fever.
Methods
Click here for a detailed description of the methods used to produce this annual report
The data used for the report were extracted from TESSy on 4 December 2015.
For 2014, 27 EU/EEA countries reported data on typhoid and paratyphoid fever. Eight countries reported data using the 2012 EU case definition for typhoid/paratyphoid fever, 13 used the 2008 definition (which does not differ from the 2012 definition), four used another definition, and two had not specified the definition used (Table 3 and Annex). Typhoid and paratyphoid fever cases could not be extracted from the datasets if countries reported aggregated data for salmonellosis (i.e. Bulgaria, Croatia and Poland).
The disease is under mandatory notification in all EU/EEA countries. The surveillance systems for typhoid/paratyphoid fever have national coverage in all but four Member States (Belgium, France, the Netherlands and Spain). The population coverage is estimated to be 30% in Spain, 48% in France and 64% in the Netherlands. The variation in coverage was taken into consideration when calculating the national notification rates. No information on estimated coverage was provided by Belgium, which prevented the calculation of notification rates. Three countries have active surveillance systems while the rest have passive surveillance. Four countries submit data from the national reference laboratory from a separate data source (not shown in Table 3).
Epidemiology
In 2014, 934 confirmed typhoid/paratyphoid fever cases were reported in 27 EU/EEA countries, resulting in an EU/EEA notification rate of 0.31 cases per 100 000 population (Table 1). Although the case numbers decreased, the rate was slightly higher than in 2013 because Italy (and its comparatively large population denominator) was excluded from the EU/EEA notification rate in 2014 due to incomplete reporting of data.
The highest notification rates in 2014 were reported by France (0.65 cases per 100 000 population), the United Kingdom (0.55 per 100 000) and Denmark (0.48 cases per 100 000) (Table 1, Figure 1). Seven countries did not report any cases of typhoid or paratyphoid fever (Cyprus, Hungary, Iceland, Latvia, Malta, Romania and Slovakia).
The majority (85%) of typhoid and paratyphoid fever cases were acquired while travelling, almost exclusively in countries outside the EU/EEA: countries in South Asia dominated the list of destinations. India, Pakistan and Bangladesh were the top three countries for travel-associated typhoid and paratyphoid fever cases. A small number of countries reported a large proportion of their cases with known travel status as domestically acquired, e.g. Greece (67%), Spain (62%) and Belgium (50%).
There was no major difference in typhoid/paratyphoid fever overall by gender (male-to-female ratio: 1.1:1). The highest notification rate (0.59 cases per 100 000 population) was reported in 5−14-year-old males, and the lowest rate was observed in ≥65-year-old women (0.09 per 100 000) (Figure 2).
There is a distinct seasonal trend for reported typhoid/paratyphoid cases (Figure 3), with a clear peak in case numbers in September and a lower peak in May. The monthly number of reported cases for 2014 was in the lowest range when compared with the previous four years, except for September 2014, where case numbers exceeded the mean. This peak was the second highest peak in the five year period 2010−2014, only exceeded by the September peak in 2010. Otherwise, a decreasing trend was observed in typhoid and paratyphoid cases in the EU/EEA during this period (Figure 4).
Threats description for 2014
No threats for typhoid and paratyphoid fever were detected in the EU/EEA in 2014.
Discussion
Typhoid and paratyphoid fever are rare infections in EU/EEA countries. Most cases (85%) are associated with travel during the incubation period, mostly to the Indian subcontinent. In the UK, which accounted for 38% of the reported cases in 2015, most of the infections were acquired by people visiting relatives in Bangladesh, India and Pakistan [1]. Infections reported in France, a country which accounted for 22% of all reported EU/EEA cases in 2015, were predominantly acquired during travel to Africa, South America and the Indian subcontinent [2]. The disease is also endemic in two of the French overseas territories, French Guiana and Mayotte. Globally, the burden of typhoid fever remains high in low- and middle-income countries, especially in South Asia [3], where the incidence in 5−15-year-olds in study sites in Pakistan and India in 2002−2004 was as high as 413 and 494 cases per 100 000 population, respectively [4]. When tested for antimicrobial susceptibility, most isolates of S. Typhi and S. Paratyphi A from South Asia were resistant to fluoroquinolones (applying the latest EUCAST clinical breakpoint), and multi-drug resistance was not uncommon [5]. In 2008, WHO recommended programmatic use of the two licensed typhoid vaccines for endemic and epidemic disease control [6]. Despite the demonstrated success of several typhoid vaccination strategies, typhoid vaccines remain underused [7].
The seasonal pattern observed in the EU/EEA, with a peak of cases in September, most likely reflects travelling during the holiday period, with disease onset after returning home.
Public health conclusions
Typhoid and paratyphoid fever are mainly travel-associated infections in the EU/EEA. Persons planning to stay in high-endemic countries for prolonged periods should consider vaccination before travelling, in line with the national recommendations.
References
- National Health Service, United Kingdom. Health topics: Typhoid fever. Leeds: NHS; 2015.
- Institut Pasteur, France. Info sheet: Typhoid and paratyphoid fever [in French]. Paris: Institut Pasteur; 2012. Available from: http://www.pasteur.fr/fr/institut-pasteur/presse/fiches-info/fievres-typhoide-et-paratyphoide. [Accessed 28 June 2016].
- Mogasale V, Maskery B, Ochiai RL, Lee JS, Mogasale VV, Ramani E, et al. Burden of typhoid fever in low-income and middle-income countries: a systematic, literature-based update with risk-factor adjustment. Lancet Glob Health. 2014;2(10):e570-80.
- Ochiai RL, Acosta CJ, Danovaro-Holliday MC, Baiqing D, Bhattacharya SK, Agtini MD, et al. A study of typhoid fever in five Asian countries: disease burden and implications for controls. Bull World Health Organ. 2008;86(4):260-8.
- Kariuki S, Gordon MA, Feasey N, Parry CM. Antimicrobial resistance and management of invasive Salmonella disease. Vaccine. 2015;33 Suppl 3:C21-9.
- World Health Organization. Typhoid vaccines – position paper. Geneva: WHO; 2008.
- Date KA, Bentsi-Enchill A, Marks F, Fox K. Typhoid fever vaccination strategies. Vaccine. 2015;33 Suppl 3:C55-61.
_________
* The European Surveillance System (TESSy) is a system for the collection, analysis and dissemination of data on communicable diseases. EU Member States and EEA countries contribute to the system by uploading their infectious disease surveillance data at regular intervals.
Confirmed cases of typhoid/paratyphoid fever: number and rate per 100 000 population, EU/EEA, 2010–2014

Reported confirmed typhoid/paratyphoid cases: notification rate per 100 000 population, EU/EEA, 2014
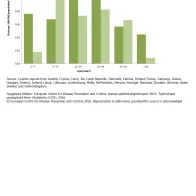
Confirmed typhoid/paratyphoid fever cases: rate per 100 000 population, by age and gender, EU/EEA, 2014

Number of confirmed cases of typhoid/paratyphoid fever by month in 2014 compared with 2010−2013, EU/EEA

Trend and number of confirmed cases of typhoid/paratyphoid fever, EU/EEA, 2010−2014
Salmonella enterica serotypes of typhoid and paratyphoid fever cases, EU/EEA, 201
Share this page
