Tularaemia - Annual Epidemiological Report 2016 [2014 data]
Tularaemia - Annual Epidemiological Report 2016
English (138.58 KB - PDF)Tularaemia, surveillance systems overview, 2014
English (24.34 KB - XLSX)Key facts
- In 2014, a total of 592 cases was reported to TESSy; 526 (88.9%) of these cases were confirmed.
- The EU/EEA notification rate in 2014 was 0.11 cases per 100 000 population.
- There was an overall increase by 70% in the number of reported confirmed cases compared with 2013.
- The highest rates were reported in middle-aged and older men.
- Sweden accounts for most of the reported cases in EU/EEA countries in 2014, followed by Hungary and Spain.
Methods
Click here for a detailed description of the methods used to produce this annual report
- In 2014, 28 EU/EEA countries provided information on tularaemia in humans.
- All reporting countries have a comprehensive surveillance system, except for the Netherlands, which did not provide any specific information. Twelve countries (Austria, Belgium, Cyprus, Greece, Iceland, Ireland, Italy, Latvia, Luxembourg, Malta, Romania and the United Kingdom) reported zero human cases.
- Twenty-two countries used the EU case definition. Germany and Italy used an alternative case definition. Belgium, Finland, France and the Netherlands did not specify their case definition or it was unknown.
- The reporting is compulsory in 25 countries, voluntary in two countries (Belgium and the United Kingdom) and ‘not specified’ for the Netherlands. The surveillance is mostly passive except in the Czech Republic and Slovakia (‘not specified’ for the Netherlands) (Annex).
Epidemiology
The overall notification rate was 0.11 per 100 000 population, higher than the rate reported in 2013 (0.06 per 100 000 population). As in the previous four years, the notification rate was highest in Sweden (1.56 per 100 000), slightly exceeding the rate of 2013 (1.13 per 100 000).The highest increase in notification rate between 2013 and 2014 was seen in Hungary (from 0.5 to 1.4 per 100 000) (Table 1).
Most of the confirmed cases in 2014 were reported by Sweden (n=150) and Hungary (n=140), followed by Spain (n=62) (figure 1). Both Hungary and Spain experienced an outbreak. Only 33% of the cases were confirmed in France and 69% in Spain in 2014.
Age and gender distribution
As in previous years, the proportion of male cases was higher (male-to-female ratio 2.5:1). The highest rates in males were observed in the 45–64-year-old group (0.21 cases per 100 000 population), followed by people 65 years and older (0.19 cases per 100 000 population). The rates among females were highest among 45–64-year-olds (0.10 cases per 100 000 population), followed by 5–14 year-olds (0.06 cases per 100 000).
Seasonality
Tularaemia shows a seasonal pattern, with most cases occurring between August and October, but some cases also occur in the winter. The 2014 peak of infections was recorded in September, which was consistent with previous years, although below the mean observed during the 2010–2013 period (Figure 3). This was mainly attributable to fewer cases in Sweden and Finland compared with the 2010–2012 period.
Discussion
Tularaemia is widely distributed throughout most of Europe and has repeatedly shown signs of local emergence and re-emergence in humans and wildlife. The disease shows clear seasonality in humans [1].
Notification rates of tularaemia vary considerably among Member States. In previous years, most cases were diagnosed in Sweden and Finland, followed by Norway, Hungary and the Czech Republic. In 2014, the majority of cases were reported by Sweden, followed by Hungary and Spain. These two countries reported an unusually high number of cases [2]. In Hungary, the increase was most likely due to an increase in the number of common voles [3].
The notification rate in Finland decreased markedly since 2012. After more than 50 years without any autochthonous case, the Netherlands reported one locally acquired human case in 2013, and in 2014, five human cases were reported at different locations; there were also three confirmed cases in hares [4]. In 2015, Germany reported three cases of tularaemia with a history of tick bites (2012 and 2013) [5].
Public health conclusions
Tularaemia is a zoonosis not transmissible from human to human [6]. Prevention consists of avoiding contact with diseased hares (skinning can be particularly infectious), wild rabbits and rodents.
There is no commercial vaccine against tularaemia, although research for the development of a vaccine is ongoing [7]. Francisella tularensis LVS (an attenuated live vaccine strain of Russian origin) can be used to prevent infections in laboratory staff and certain other professional groups (hunters, trappers), but it is not routinely accessible.
Data on tularaemia surveillance in animals in European are available from a joint ECDC/EFSA report [8].
References
- Hestvik G, Warns-Petit E, Smith LA, Fox NJ, Uhlhorn H, Artois M, et al. The status of tularemia in Europe in a one-health context: a review. Epidemiol Infect. 2015 Jul;143(10):2137-60.
- Luque-Larena JJ, Mougeot F, Roig DV, Lambin X, Rodriguez-Pastor R, Rodriguez-Valin E, et al. Tularemia outbreaks and common vole (Microtus arvalis) irruptive population dynamics in northwestern Spain, 1997–2014. Vector Borne Zoonotic Dis. 2015 Sep;15(9):568-70.
- Maurin M, Gyuranecz M. Tularaemia: clinical aspects in Europe. Lancet Infect Dis. 2016 Jan;16(1):113-24.
- Rijks JM, Kik M, Koene MG, Engelsma MY, van Tulden P, Montizaan MG, et al. Tularaemia in a brown hare (Lepus europaeus) in 2013: first case in the Netherlands in 60 years. Euro Surveill. 2013;18(49).
- Boone I, Hassler D, Nguyen T, Splettstoesser WD, Wagner-Wiening C, Pfaff G. Tularaemia in southwest Germany: Three cases of tick-borne transmission. Ticks Tick Borne Dis. 2015 Jul;6(5):611-4.
- European Centre for Disease Prevention and Control. Tularaemia: factsheet for health professionals.
- Marohn ME, Barry EM. Live attenuated tularemia vaccines: recent developments and future goals. Vaccine. 2013 Aug 2;31(35):3485-91.
- EFSA (European Food Safety Authority), ECDC. The European Union summary report on trends and sources of zoonoses, zoonotic agents and foodborne outbreaks in 2014. EFSA Journal 2015;13(12):4329. doi:10.2903/j.efsa.2015.4329. Available from: https://ecdc.europa.eu/en/european-union-summary-report-trends-and-sources-zoonoses-zoonotic-agents-and-food-borne-7
_________
* The European Surveillance System (TESSy) is a system for the collection, analysis and dissemination of data on communicable diseases. EU Member States and EEA countries contribute to the system by uploading their infectious disease surveillance data at regular intervals.
Confirmed tularaemia cases: number and rate per 100 000 population, EU/EEA, 2010–2014
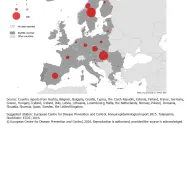
Number of confirmed tularaemia cases, EU/EEA, 2014

Confirmed tularaemia cases, by age and gender, EU/EEA, 2014

Seasonal distribution of confirmed tularaemia cases, EU/EEA, 2014 compared with 2010−2013
Share this page
