Salmonellosis - Annual Epidemiological Report 2016 [2014 data]
Salmonellosis - Annual Epidemiological Report 2016
English (172.44 KB - PDF)Key facts
- Salmonellosis is the second most commonly reported gastrointestinal infection and an important cause of foodborne outbreaks in the EU/EEA.
- In 2014, 89 883 laboratory-confirmed cases were reported; the EU/EEA notification rate was 25.4 cases per 100 000 population.
- Reported salmonellosis case numbers continued to decrease in the EU/EEA. This decrease is mainly attributed to the implementation of successful Salmonella control programmes, particularly in poultry production.
- The reported case rate was highest in young children 0−4 years of age: 115.7 cases per 100 000 population were reported in 2014 − six times higher than in adults.
- Clusters of cases with the outbreak strain belonging to S. Stanley serotype continued to occur in 2014; the peak of the outbreak, linked to contamination in the turkey production chain, was in 2012.
Methods
Click here for a detailed description of the methods used to produce this annual report
The data used for this report were extracted from TESSy on 4 December 2015.
In 2014, 30 EU/EEA countries reported data on salmonellosis. Twenty-four countries reported data using either the 2008 or the 2012 EU case definition for salmonellosis, which is essentially the same. Four countries used another definition, and two did not specify the definition used. The disease is under mandatory notification in 25 countries, voluntary in four, and one country has another type of surveillance system. The surveillance systems for salmonellosis have national coverage in all Member States except in Belgium, France, the Netherlands and Spain. The population coverage is estimated to be 30% in Spain, 48% in France and 64% in the Netherlands. The variation in coverage was taken into consideration when calculating the notification rates. No information on estimated coverage was provided by Belgium, thus no notification rates were calculated. Three countries have active surveillance systems while the rest have passive systems. Twenty countries have surveillance systems which integrate laboratory and epidemiological data, and four countries submit data from the national reference laboratory via a separate data source.
In addition to case-based surveillance, ECDC coordinates molecular typing-enhanced surveillance on salmonellosis through isolate-based data collection. A typing-based multi-country cluster of Salmonella spp. is currently defined as at least two different countries reporting at least one isolate each with matching XbaI pulsotypes, or matching multiple locus variable-number of tandem repeat analysis (MLVA) types for Salmonella enterica serovar Typhimurium, no more than eight weeks apart.
Epidemiology
In 2014, 91 408 salmonellosis cases were reported by 30 EU/EEA countries, with 89 883 confirmed cases and an EU/EEA notification rate of 25.4 cases per 100 000 population (Table 1). Compared with 2013 (21.4 cases per 100 000), this represented a 19% increase in the EU/EEA notification rate, which was affected by Croatia reporting confirmed cases for the first time in 2014 and Italy being excluded from EU/EEA rate calculations due to incomplete reporting in 2014.
The highest case rate of salmonellosis was observed among young children 0-4 years of age, with 128.9 cases per 100 000 population (Figure 2). The rate in young children was almost three times higher than in older children and at least six times as high as in the remaining age groups. In some countries, the rate among young children was more than 30 times higher than that among adults 25−44 years of age, i.e. Bulgaria (32 times), Cyprus (60 times), Greece (40 times), and Portugal (82 times). In these countries, the proportions of hospitalised cases were very high in all age groups (average 77−85%, no data available for Bulgaria) while the salmonellosis notification rates were low. There were no differences in the overall rates between males and females (male−female ratio 1.0:1.0).
There is a clear seasonal variation in the number of reported salmonellosis cases (Figure 3), with case numbers increasing over the summer months, peaking in August and September, and then decreasing. In 2014, the summer peak was slightly less pronounced than in the previous four years.
There was a decreasing trend of salmonellosis in the EU/EEA in the five-year period 2010−2014 (Figure 4).
Molecular typing-enhanced surveillance
In 2014, 16 countries submitted Salmonella typing data, based on which 51 molecular typing cluster investigations (MTCIs) were initiated, ten based on pulsotypes and 41 using MLVA. Two of the MTCIs were escalated to ‘urgent inquiries’ and one of the two was covered by an ECDC rapid risk assessment. The three most commonly reported reference types were S. Typhimurium MLVA types 3-12-9-NA-211, 3-13-9-NA-211 and 3-14-9-NA-211.
Threats description for 2014
Following the multi-country outbreak of S. Stanley in the EU linked to contamination in the turkey production chain in 2011–2012, cases peaked in 2012 and then decreased in 2013. In 2014, cases of S. Stanley remained at a higher level than before the outbreak and several clusters of cases with the outbreak strain were reported, suggesting that the strain was still circulating in the European food market [1]. This demonstrated the long-lasting public health impact that substantial contamination by any Salmonella serotype at the farm level can have in the EU.
The highest notification rates in 2014 were reported by the Czech Republic (126.1 cases per 100 000 population) and Slovakia (75.3), followed by Hungary (53.1) and Spain (47.5) (Table 1 and Figure 1). The lowest rates were reported by Portugal and Greece (≤4.0 per 100 000). The large increase in notification rate in the Czech Republic was accompanied by an increase in the number of Salmonella outbreaks in 2014. This was also seen in Slovenia where nine Salmonella outbreaks were reported from April to October 2014; eight were foodborne and caused by Salmonella Enteritidis and one was waterborne caused by Salmonella Typhimurium. In Spain, improved coverage of the surveillance system for salmonellosis in 2014 resulted in an increase in reported cases and notification rate.
The proportion of domestic cases versus travel-associated cases varied markedly between countries, with the highest proportions of domestic cases ranging from 81.5% to 99.9% in the Czech Republic, Estonia, Germany, Greece, Hungary, Latvia, Malta, the Netherlands and Slovakia. The highest proportions of travel-related cases were reported by three Nordic countries (Finland, Norway and Sweden), where more than 70% of the cases were classified as travel-related.
Discussion
The rate of salmonellosis reported in young children was six times as high as among adults. This may be due to the higher proportion of symptomatic infections among the young, as well as an increased likelihood for parents to bring their children to the doctor and doctors to request samples from small children. The substantial difference between the rates in young children and adults observed in some countries is most likely also affected by underreporting of cases. This is supported by the high proportion of hospitalised cases reported in these countries for a disease which in most cases causes mild symptoms, while at the same time very low notification rates of Salmonella infections are reported. A large European study on salmonellosis seroincidence concluded that seroincidence was not correlated with the reported national incidence of Salmonella infections but rather correlated with prevalence data of Salmonella in laying hens, broilers and slaughter pigs, as assessed in the EFSA EU baseline surveys [2]. Seroincidence also correlated with Swedish data on the country-specific risk of travel-associated salmonellosis [2]. While it is unrealistic that surveillance systems could capture all cases of mild disease, improvements in national surveillance systems could reduce underreporting so it would eventually reach similar levels across all EU/EEA countries. This would require extensive work at all levels, with significant costs associated.
Over the last eight years, EU Member States showed a statistically significant decreasing trend in salmonellosis cases and in the reported number of foodborne outbreaks due to Salmonella [3]. This decrease is thought to be connected with the implementation of Salmonella control programmes in the poultry industry, particularly in laying hens and broilers [4]. Nonetheless, salmonellosis remains the second most common zoonosis in humans in the EU. In 2014, Salmonella was surpassed for the first time by foodborne viruses as the most common cause of foodborne outbreaks [4] although this could also reflect improved virus detection methods from stool and food isolates. Salmonella accounted for 1 048 foodborne outbreaks in 2014, corresponding to 20% of all reported foodborne outbreaks, and eggs and egg products continued to be the most commonly identified vehicle in these outbreaks [3].
The reduction targets for specific Salmonella serotypes in targeted animal populations clearly had an effect on the prevalence of those serotypes, e.g. of S. Enteritidis and S. Typhimurium in broilers and turkey [3], which is also reflected in fewer human cases with these serotypes. Non-targeted serotypes are however not being reduced to the same extent. A steady increase of S. Infantis has been observed in broiler and turkey in the last years [3]. Also, in animal groups where no target is set, increasing numbers of positive Salmonella findings have been reported, e.g. for S. Typhimurium in pigs [4]. National or multinational outbreaks involving other serotypes than the two most common ones (S. Enteritidis and S. Typhimurium) occur every year. Examples in 2014 were the continued S. Stanley outbreak linked to the turkey production chain, a national outbreak of S. Muenchen linked to consumption of raw pork products, and an outbreak of cases of S. Chester linked to travel to a non-EU country [4]. Multidrug-resistant and/or high ciprofloxacin-resistant clones of e.g. S. Kentucky, S. Stanley and S. Infantis are also spreading in the animal and human population in the EU [5].
Public health conclusions
The rates of salmonellosis vary between EU/EEA countries, reflecting differences in, for example, prevalence in food-production animals, food and animal trade between countries, the proportion of travel-associated cases, and the quality and coverage of surveillance systems. While salmonellosis is decreasing in the EU/EEA due to control programmes targeting specific serotypes in the animal population, it is important to point out that all other Salmonella serotypes in food animals should also be acted upon since they can cause infections in humans and result in outbreaks.
References
1. European Food Safety Authority and European Centre for Disease Prevention and Control. Multi-country outbreak of Salmonella Stanley infections – Third update, 8 May 2014. Stockholm and Parma: ECDC/EFSA; 2014.
2. Mølbak K, Simonsen J, Jørgensen CS, Krogfelt KA, Falkenhorst G, Ethelberg S, et al. Seroincidence of human infections with nontyphoid Salmonella compared with data from public health surveillance and food animals in 13 European countries. Clin Infect Dis. 2014 Dec 1;59(11):1599-606.
3. European Food Safety Authority and European Centre for Disease Prevention and Control. The European Union summary report on trends and sources of zoonoses, zoonotic agents and foodborne outbreaks in 2014. EFSA Journal 2015;13(12):4329.
4. Hugas M, Beloeil PA. Controlling Salmonella along the food chain in the European Union – progress over the last ten years. Euro Surveill. 2014;19(19).
5. European Food Safety Authority and European Centre for Disease Prevention and Control. The European Union summary report on antimicrobial resistance in zoonotic and indicator bacteria from humans, animals and food in 2014. EFSA Journal 2016;14(2):4380. Available from: http://ecdc.europa.eu/en/publications/Publications/antimicrobial-resistance-zoonotic-bacteria-humans-animals-food-EU-summary-report-2014.pdf
_________
* The European Surveillance System (TESSy) is a system for the collection, analysis and dissemination of data on communicable diseases. EU Member States and EEA countries contribute to the system by uploading their infectious disease surveillance data at regular intervals.
Reported confirmed salmonellosis cases: number and rate per 100 000 population, EU/EEA, 2010–2014

Reported confirmed non-typhoidal salmonellosis cases: rate per 100 000 population, EU/EEA, 2014
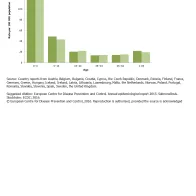
Reported confirmed non-typhoidal salmonellosis cases: rate per 100 000 population, by age and gender, EU/EEA, 2014

Non-typhoidal salmonellosis cases: seasonal distribution, EU/EEA, 2014 compared with 2009−2013

Reported confirmed non-typhoidal salmonellosis cases: trend and number, EU/EEA, 2010−2014
Share this page
