Botulism - Annual Epidemiological Report, 2016 [2014 data]
Botulism - Annual epidemiological report 2016
English (120.42 KB - PDF)Botulism, surveillance systems overview, 2014
English (24.19 KB - XLSX)Key facts
-
In 2014, 123 cases of botulism were reported by 16 EU/EEA countries, including 91 cases reported as confirmed. Thirteen countries notified zero cases.
-
The notification rate was 0.02 cases per 100 000 population.
- Romania notified the highest number of cases (N=31) and presented the highest rate (0.15 cases per 100 000 population).
Methods
Click here for a detailed description of the methods used to produce this annual report
- In 2014, 29 countries reported data, including 13 countries that reported zero cases.
- Nine countries reported in accordance with the 2012 EU case definition, 13 countries used the 2008 EU case definition, and the remaining seven countries used other case definitions.
- Botulism is a mandatorily notifiable disease in all reporting countries.
Epidemiology
In 2014, 123 cases were reported, including 91 confirmed cases, by a total of 16 EU/EEA countries. Thirteen countries had no cases. Italy and Liechtenstein had not reported data for 2014 at the time of the data extraction. The EU/EEA notification rate was 0.02 cases per 100 000 population (Table 1).
Romania (31 confirmed cases), Poland (17) and Hungary (12) were the countries accounting for most of the confirmed cases. Twelve countries reported between one and six confirmed cases each.
Romania (0.15 cases per 100 000), Hungary (0.12 cases per 100 000) and Lithuania (0.10 cases per 100 000) reported the highest rates in 2014 (Table 1).
With 67 confirmed cases in males and 35 in females, the male-to-female ratio was 1.9:1 in 2014. The most affected age groups were 0–4- and 45–65-year-old males, and 0–4- and 25–44-year-old females (Figure 1).
While in 2014, the highest number of cases was reported in July, the data from previous years show no seasonality but irregular, random peaks (Figure 2). Figure 3 shows the secular trend for EU/EEA countries.
Threats description for 2014
An outbreak of botulism among injecting drug users in Norway and Scotland started in December 2014. By February 2015, 23 cases of botulism had been reported [1]. The source of the infection was assumed to be contaminated heroin.
Discussion
Figure 3 shows an ascending trend in the rate of botulism notifications in the EU/EEA after July 2012. This observation is based on a small number of cases and does not necessarily represent a real increase in incidence.
The randomly occurring peaks may be explained by small-scale outbreaks due to locally produced food. Botulism cases are often detected as sporadic cases which may belong to household clusters. Case reports and retrospective analyses of cases are useful and complement the mandatory surveillance systems [2,3].
Public health conclusions
While the case definition for surveillance at the EU level focuses on C. botulinum as the etiological agent, sporadic clusters and cases due to type F toxin produced by C. baratii have been reported in recent years [4,5]. These botulism cases due to F toxin type are a cause of concern because the antitoxin is not readily available in Europe, and the commonly used antitoxins may not effectively neutralise toxin F. Preparedness plans may need to consider the timely access to antitoxins in order to cover a broad range of different toxin types, including toxin F [4,5]. In addition, subtyping of botulism neurotoxins is important to monitor the evolution of strains and its implications for public health as exemplified by the recent characterisation of a novel botulism neurotoxin subtype (BoNT/A8) in Germany [6].
References
- European Centre for Disease Prevention and Control. Wound botulism in people who inject heroin, Norway and the United Kingdom – 14 February 2015. Stockholm: ECDC; 2015. Available from: http://www.emcdda.europa.eu/system/files/publications/856/09-02-2015-RRA-Botulism-Norway%2C%20United%20Kingdom.pdf.
- Ambrožová H, Džupová O, Smíšková D, Roháčová H. Familial occurrence of botulism – A case report. Klinicka Mikrobiologie a Infekcni Lekarstvi. 2014;20(2):40-2.
- Lonati D, Flore L, Vecchio S, Giampreti A, Petrolini VM, Anniballi F, et al. Clinical management of foodborne botulism poisoning in emergency setting: An Italian case series. Clinical Toxicology. 2015;53(4):338.
- Castor C, Mazuet C, Saint-Leger M, Vygen S, Coutureau J, Durand M, et al. Cluster of two cases of botulism due to Clostridium baratii type F in France, November 2014. Euro Surveill. 2015;20(6):pii=21031.
- European Centre for Disease Prevention and Control. Scientific advice on type F botulism. Stockholm: ECDC; 2015.
- Kull S, Schulz KM, Weisemann J, Kirchner S, Schreiber T, Bollenbach A, et al. Isolation and functional characterization of the novel Clostridium botulinum neurotoxin A8 subtype. PLoS One. 2015;10(2):e0116381.
_________
* The European Surveillance System (TESSy) is a system for the collection, analysis and dissemination of data on communicable diseases. EU Member States and EEA countries contribute to the system by uploading their infectious disease surveillance data at regular intervals.
Source: Country reports. Legend: Y = yes, N = no, C = case based, A = aggregated, · = no data reported, ASR: agestandardised rate, = no report
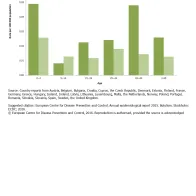
Source: Country reports from Austria, Belgium, Bulgaria, Croatia, Cyprus, the Czech Republic, Denmark, Estonia, Finland, France, Germany, Greece, Hungary, Iceland, Ireland, Latvia, Lithuania, Luxembourg, Malta, the Netherlands, Norway, Poland, Portugal, Romania, Slovakia, Slovenia, Spain, Sweden, the United Kingdom.
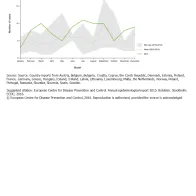
Source: Country reports from Austria, Belgium, Bulgaria, Croatia, Cyprus, the Czech Republic, Denmark, Estonia, Finland, France, Germany, Greece, Hungary, Iceland, Ireland,
Latvia, Lithuania, Luxembourg, Malta, the Netherlands, Norway, Poland, Portugal, Romania, Slovakia, Slovenia, Spain, Sweden.
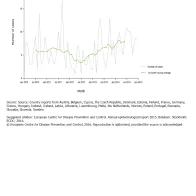
Source: Country reports from Austria, Belgium, Bulgaria, Croatia, Cyprus, the Czech Republic, Denmark, Estonia, Finland, France, Germany, Greece, Hungary, Iceland, Ireland,
Latvia, Lithuania, Luxembourg, Malta, the Netherlands, Norway, Poland, Portugal, Romania, Slovakia, Slovenia, Spain, Sweden.
Share this page
